Healthy Teeth, Happy Life.
Severe Night Toothache & Deep Cavity Treatment in California, US
Severity:
Teeth Problems:
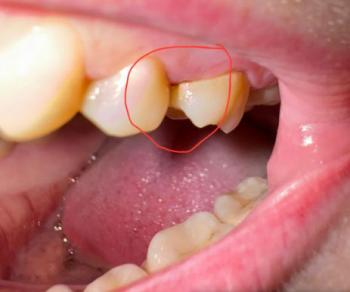
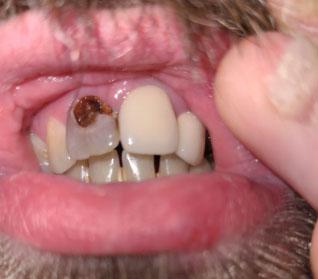
The image strongly suggests a case of Severe Tooth Decay and Possible Pulp Exposure. The pain shown in the right panel indicates a severe toothache, which often means the decay has progressed to the innermost part of the tooth (the pulp), causing irreversible pulpitis or a dental abscess. This requires urgent professional attention.
Do not attempt to self-treat this condition. Use the provided directory link to find a nearby clinic immediately.
Analysis and Likely Diagnosis Based on Image
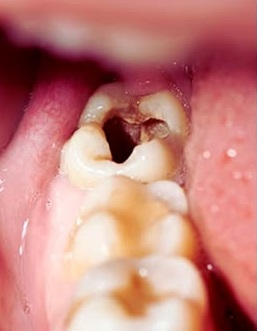
The magnified image of the tooth (left panel) clearly shows:
-
Extensive Cavity: A very large, dark, and deep hole (cavity or caries) is visible on the chewing surface (occlusal) of the molar.
-
Dentin/Pulp Involvement: The depth of the decay appears to reach or nearly reach the pulp chamber, which contains the nerves and blood vessels. This explains the severe, spontaneous night pain depicted on the right.
Possible Diagnoses:
-
Irreversible Pulpitis: Inflammation of the dental pulp that won't heal. This requires Root Canal Treatment (RCT) or extraction.
-
Periapical Abscess: An infection at the tip of the tooth root, often a complication of irreversible pulpitis. This would require RCT or extraction, plus draining the infection.
-
Necrotic Pulp: The nerve tissue inside the tooth has died. This also requires RCT or extraction.
Recommended Process to Execute
The process is generally structured in two phases: Emergency Relief and Definitive Treatment.
-
Immediate Action:
-
Visit a Clinic: Use the provided directory link: https://cebudentalimplants.com/map-dental-clinic to locate the nearest dental clinic immediately.
-
-
Clinical Examination & Diagnosis:
-
Consultation: Dentist will review symptoms (especially pain severity and duration).
-
X-ray (Radiograph): Crucial for determining the depth of decay, assessing the condition of the roots, and checking for a periapical abscess (infection at the bone level).
-
Pulp Testing: Tests (like cold or electric pulp test) to determine if the nerve is vital, irreversibly inflamed, or necrotic (dead).
-
-
Definitive Treatment:
-
Option 1: Root Canal Treatment (RCT): If the tooth is salvageable, the infected pulp is removed, the canals are cleaned and sealed, and the tooth is restored, usually with a dental crown for strength.
-
Option 2: Extraction: If the decay is too extensive, the tooth structure is severely compromised, or the infection is too widespread, the tooth may need to be removed (extracted). This would require subsequent replacement (e.g., a dental implant, bridge, or partial denture).
-
Time Frame and Scaling Issues
Time Frame to Heal:
The healing time depends entirely on the treatment:
-
Extraction: Physical healing of the socket takes 7-10 days for the initial clot to stabilize, but the bone takes several months.
-
Root Canal Treatment (RCT): The actual RCT is often completed in 1-2 visits. Initial symptoms subside within 2-3 days. Full final restoration (placing the crown) can take 1-3 weeks after the root canal is finished.
Issue That Will Scale Up (If it takes 14 days without treatment):
If this condition is left untreated for 14 days or longer, the primary issue that will scale up is infection spread and systemic risk:
-
Increased Pain: The pain will become more intense, widespread, and resistant to over-the-counter pain medication.
-
Abscess Formation: The infection will likely progress from a localized pulp infection to a full-blown dental abscess with swelling in the jaw, cheek, or neck.
-
Bone Loss: Chronic infection causes destruction of the surrounding jawbone (periapical rarefaction).
-
Systemic Infection (The Major Concern): The most serious issue is the infection spreading to other parts of the body. In severe cases, this can lead to cellulitis (a dangerous soft-tissue infection), Ludwig's Angina (life-threatening neck/floor-of-mouth swelling), or even sepsis (blood poisoning).