From Pain to Perfect — We Care for Your Smile.
Emergency Dental Appointment for Failed Crown or Deep Cavity
Severity:
Teeth Problems:
Initial Image Analysis
-
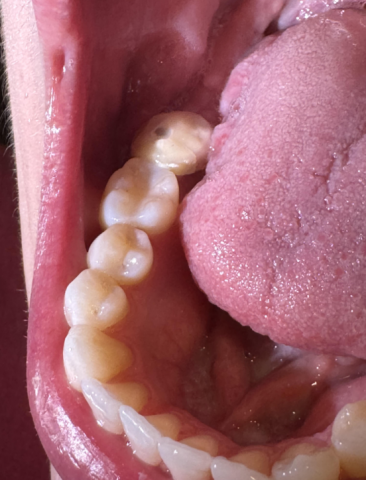
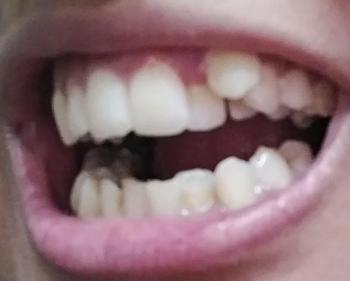
Image Observations: The picture shows the lower right side of the mouth (Mandibular quadrant).
-
The tooth farthest back (most posterior) appears to have a restoration (filling or inlay/onlay) or possibly a crown which exhibits a large, dark, and deep-looking defect or void on its biting surface (occlusal surface). The defect appears dark brown/black with a distinct border.
-
The adjacent tooth (second molar/premolar) also shows signs of an existing white or tooth-colored filling (composite or glass ionomer) with some possible discoloration or breakdown at the margins.
-
The surrounding soft tissues (gums and tongue) appear generally healthy.
-
-
Client Statement: "Does my crown implant look normal?"
-
Clarification: It is most likely that the question refers to a crown placed on a natural tooth, or a restoration on a natural tooth. A dental implant would typically have a crown cemented on an abutment, and the visible issue appears to be within the structure of the tooth/crown itself.
-
Full Analysis and Potential Diagnosis
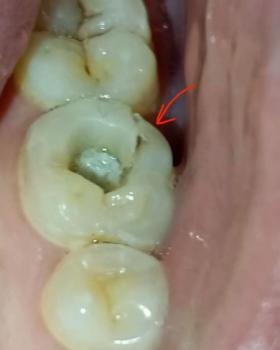
The primary concern is the large, dark defect on the most posterior tooth.
| Potential Issue | Deep Examination | Scaling/Issue Escalation |
| 1. Secondary Caries (Decay) | The most likely diagnosis. Decay has formed around or under the existing restoration (crown/filling) due to marginal leakage. The dark color is staining combined with the decaying dentin. The defect appears very deep, possibly nearing the pulp chamber (nerve). | High Risk. If this is active decay, it will rapidly reach the pulp (nerve), especially within a 14-day timeframe or less given its depth. This progression leads to pulpitis, which can be irreversible and cause severe pain, abscess formation, and require Root Canal Treatment or Extraction. |
| 2. Failed/Fractured Restoration | The restoration itself (filling or crown material) has fractured, leaving a deep hole that is now stained with food and plaque. | Moderate Risk. While the material is fractured, the exposed tooth structure is highly vulnerable to rapid decay (Secondary Caries - see #1) and sensitivity. |
| 3. Arrested Stain/Pigmentation | Highly unlikely given the size and depth. This would be a stable, deep stain or a dark-colored restorative material (like silver amalgam) that has fractured. | Low Risk. Only if the material is stable. If it's a fractured filling (Amalgam), it must be replaced to prevent decay. |
Time Frame to Heal
-
This condition will not heal on its own. It requires clinical intervention.
-
Time Frame to Scale Up: Given the apparent depth of the defect, the condition could escalate from asymptomatic or mild sensitivity to a severe, painful pulp infection (requiring root canal) within 14 days.
Process to Execute (By a Dentist)
-
Clinical/Visual Exam: The dentist will use a dental explorer to confirm the depth and softness of the defect and assess the integrity of the restoration margins.
-
Radiographs (X-rays): A periapical or bitewing X-ray is mandatory to determine:
-
The exact depth of the lesion relative to the pulp.
-
Whether there is any bone loss or periapical radiolucency (infection at the root tip).
-
If the tooth is supported by an implant or is a natural tooth.
-
-
Treatment Options:
-
If not pulp-involved: Removal of the failed restoration and all decayed material, followed by placement of a new, larger filling or a full crown.
-
If pulp-involved: Root Canal Treatment must be performed first, followed by a core build-up and then a new crown.
-
If severely compromised: The tooth may require Extraction.
-
Comments
The defect on the posterior tooth is not normal and appears to be a severe case of decay or restoration failure. Immediate consultation is strongly advised.