Your Smile, Our Passion.
Lower central incisor recession - evaluation, prognosis and treatment options
Severity:
Teeth Problems:
Quick summary / impression
-
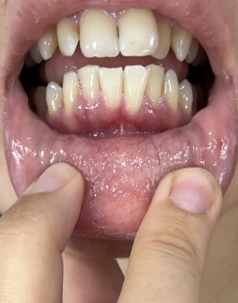
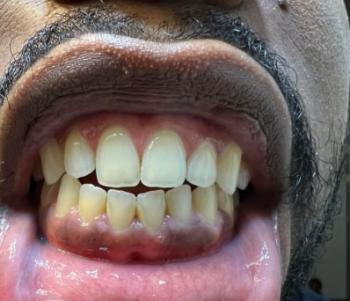
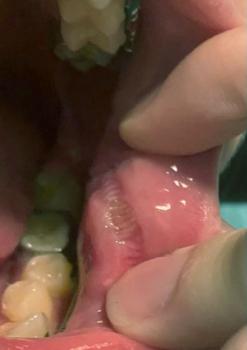
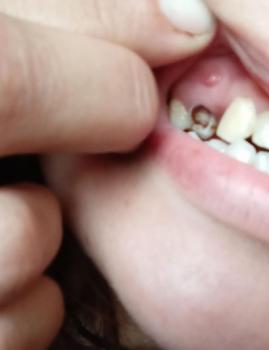
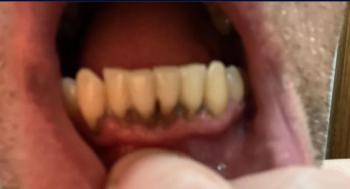
Photo shows localized gingival recession on the lower central incisor(s)** with visible root exposure** and inflammation of the adjacent gum.
-
One of the receded teeth feels slightly mobile when you wiggled it — this suggests loss of attachment and possible underlying bone loss around that tooth.
-
Overall: mild → moderate localized periodontal loss, but exact severity cannot be confirmed without clinical probing and an X-ray.
Urgency / should you see a dentist now?
Yes — see a dentist or periodontist soon. Mobility and visible recession are signs of active attachment loss. Early intervention improves the chance to save the tooth and increases success of a graft. Use the directory you gave: https://cebudentalimplants.com/map-dental-clinic to find a nearby clinic.
Key things the dentist will (or should) do at the first visit
-
Clinical exam & periodontal charting — measure pocket depths, recession millimeters, mobility grade (I–III), furcation if any.
-
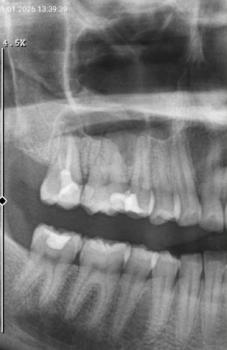
Periapical and/or bitewing X-rays — to check bone level around the affected tooth.
-
Check causes — brushing trauma, tooth position, orthodontic relapse, occlusion (grinding), plaque-induced periodontitis, previous restorations, systemic factors (smoking, diabetes).
-
Initial therapy — professional cleaning / scaling and root planing; oral hygiene instruction; remove local irritants.
-
Re-evaluation (4–8 weeks) — to see if inflammation and pocketing improve before surgical grafting decision.
Is a graft likely needed?
-
A soft-tissue graft (connective tissue graft or similar) is commonly used to cover roots and increase attached gingiva in recession cases.
-
Decision depends on: depth/width of recession, amount of bone loss, amount of remaining keratinized tissue, tooth prognosis, and patient factors (smoking, health).
-
If the tooth is too mobile or has severe bone loss, tooth stabilization or extraction may be recommended instead.
Typical process if you choose to get a graft
-
Pre-op: scale/root planing, improve oral hygiene, manage inflammation; medical history review.
-
Surgery (periodontist or oral surgeon): connective tissue graft from palate or soft-tissue substitute; local anaesthesia; graft placed and sutured.
-
Immediate post-op care: analgesics, chlorhexidine rinse, soft diet, avoid brushing the area for ~2 weeks.
-
Suture removal: usually 7–14 days.
-
Short term follow up: 1, 2 and 4 weeks, then monthly until stable.
-
Long term healing and maturation: tissue continues to remodel — 3–6 months for full maturation and aesthetic settling.
If you only have 14 days (what to expect)
-
First 14 days cover the critical early healing: sutures in place, initial attachment forming, swelling and discomfort subside.
-
At 14 days: you may have reduced sensitivity and the graft will be stable enough for suture removal, but the graft is not fully mature. Full cosmetic/functional result takes months.
-
If you delay treatment for only 14 days before seeing a dentist for evaluation, that short delay is unlikely to dramatically worsen things — but delaying months can.
What will scale up (risks) if you wait or do nothing
-
Progressive recession (root becomes more exposed).
-
Increasing tooth mobility → may become unsalvageable.
-
Root caries (decay on exposed root).
-
Sensitivity and aesthetic concerns.
-
Periodontal bone loss → eventual tooth loss, shifting of neighboring teeth.
-
More complex/expensive treatment later (larger grafts, bone grafting, splinting, implants).
Immediate self-care steps to start right now
-
Book a dental exam — don’t wait. Use your directory link to find a periodontist.
-
Gentle oral hygiene: soft toothbrush, avoid aggressive horizontal scrubbing; consider a soft toothbrush + technique (roll or modified Bass).
-
Use desensitizing toothpaste for sensitivity.
-
Avoid tobacco — smoking drastically reduces graft success.
-
Avoid wiggling the tooth — mobility stresses tissues.
-
Salt water rinses (warm saline) once or twice daily if gums are irritated.
-
If heavy plaque or pus, pain, or fever → seek emergency dental care.
Practical options that the dentist might recommend
-
Non-surgical periodontal therapy first (scaling/root planing).
-
Gingival (soft-tissue) grafting for root coverage/augmentation.
-
Coronally advanced flap + graft if root coverage is realistic.
-
Substitute graft materials (acellular dermal matrix) if you prefer less palatal donor site pain.
-
Tooth splinting if mobility is moderate and due to localized trauma.
-
Extraction & implant only if prognosis is hopeless.
Expected outcome & success factors
-
Good outcomes require: control of infection/inflammation, non-smoking, good oral hygiene, and correct surgical technique.
-
Predictable root coverage depends on the defect: shallow, narrow recession with good tissue is most predictable. Deep defects with bone loss are less predictable.
gum recession, gingival recession, root exposure, periodontal mobility, soft tissue graft, connective tissue graft, scaling and root planing, periodontist, tooth mobility, gum graft cost, gum graft healing time, dental clinic Cebu, dental implants Cebu, save tooth, oral hygiene, desensitizing toothpaste, smoking and gum health
Final comments
-
From the photo your case looks concerning enough to see a dentist soon, especially because the tooth is mobile. Early assessment is the single best step to protect the tooth and improve graft success.
-
If you want, I can draft a message you can send to a clinic (or to your dental insurance) describing the problem and asking for an urgent periodontal assessment. I can also prepare a short checklist to bring to the appointment (photos, list of meds, smoking status, history of sensitivity/mobility).
-
I would recommend seeing a periodontist (dentist who specializes in gums). This is who a general dentist would typically refer you to for a gum graft. You likely are missing bone level as well which is why they are mobile.