Your Smile, Perfected with Precision.
Extraction of Ectopic Nasal/Erupting 21 in a 7-Year-Old — Post-op Care and 14-Day Risk Management
Severity:
Teeth Problems:
Short summary / likely scenario
-
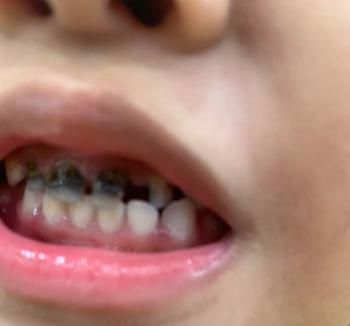
A 7-year-old male with an ectopically erupting/extruded permanent tooth (FDI 21) that presented in or near the nasal cavity/vestibule and was extracted.
-
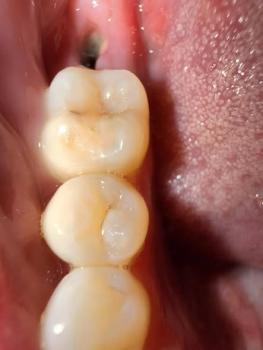
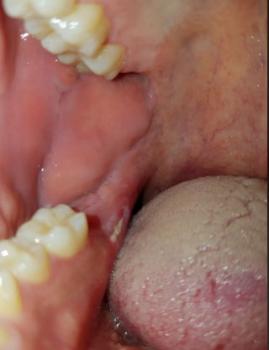
Photo shows the nostril/oral vestibule area with the extraction site and adjacent mucosa — looks like soft-tissue involvement of the nose/nasal floor region rather than a simple intraoral socket alone.
-
Because this involves the nasal mucosa / floor of nose, management and follow-up should consider both dental and ENT issues.
Examination (based on the photo + history)
-
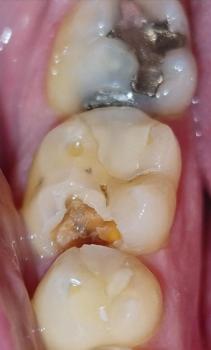
Local soft tissue defect/laceration near the nasal vestibule — extraction site appears fresh.
-
No active heavy bleeding visible in photo (good). Mild blood clot/serous exudate likely present.
-
Possible communication risk between oral cavity and nasal floor depending on defect depth — needs direct clinical check.
-
Age 7: root development of permanent central incisor may be incomplete — consider risk to adjacent developing tooth buds.
Healing timeline & what to expect
Day 0–3 (immediate):
-
Clot formation, soft tissue swelling, mild nasal discomfort. Minimal serosanguinous discharge possible.
-
Patient should avoid nose blowing, vigorous sneezing, and digital trauma.
Day 4–14 (first two weeks — critical):
-
Soft tissue epithelialization begins; reduction in swelling and pain.
-
Sutures (if placed) typically removed at 7–10 days. By day 14 most soft tissue should look significantly healed though mucosa may still be fragile.
1–3 months:
-
Deeper soft tissue maturation and bone apposition. Monitor for persistent fistula or sinus symptoms.
3–6 months+:
-
Full remodelling of alveolus and confirmation that no chronic nasal communication or infection persists.
Post-op care / process to execute (practical steps)
-
Immediate care (first 48–72 hrs):
-
Apply gentle external pressure if bleeding; avoid nose blowing.
-
Cold compress intermittently for first 24 hrs for swelling.
-
Soft diet; avoid inserting anything into nostril.
-
-
Medications (as indicated by clinician):
-
Analgesics (paracetamol/ibuprofen per paediatric dosing).
-
Consider short course of systemic antibiotics if contamination, large mucosal tear, or ENT/dental surgeon prescribes (amoxicillin ± clavulanate or per local guidelines).
-
Nasal saline sprays to keep mucosa moist (once bleeding controlled).
-
-
Wound care & behaviour:
-
No nose blowing for 7–14 days; sneeze with mouth open.
-
Keep child from rubbing/picking the area.
-
-
Follow-up:
-
24–72 hr check (to ensure hemostasis and assess early infection).
-
7–10 day suture check/remove.
-
2-week and 1-month review to confirm epithelialization and screen for oro-nasal fistula.
-
ENT referral if any nasal obstruction, unilateral nasal discharge, or signs of sinus involvement.
-
-
Radiographic follow-up:
-
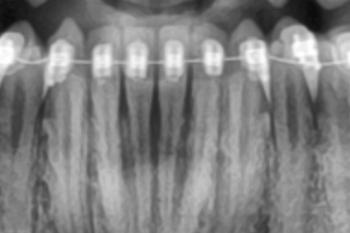
Periapical/panoramic radiograph or CBCT if retained fragments / concern for adjacent developing tooth bud.
-
If healing is only 14 days — potential issues that can scale up
(If the site still problematic at day 14, be alert for:)
-
Persistent oro-nasal communication (fistula) → chronic nasal regurgitation, speech issues, recurrent infection.
-
Infection / sinusitis (unilateral purulent nasal discharge, fever) → needs antibiotics/ENT drainage if severe.
-
Delayed soft tissue closure → may require secondary surgical closure (local flaps).
-
Pulpal / developmental damage to adjacent developing permanent teeth → arrested root development, discoloration, or need for future endodontic/orthodontic care.
-
Retained root fragment → persistent inflammation or sinus tract requiring removal.
-
Psychological/behavioural issues — children may pick at site; increases risk for failure.
Red flags — seek immediate re-evaluation if any of these occur
-
Increasing pain, swelling, fever.
-
Continuous or worsening nasal discharge (especially purulent or foul-smelling).
-
Persistent bleeding not controlled by simple measures.
-
Difficulty breathing or severe nasal obstruction.
-
Signs of oral–nasal regurgitation of liquids.
Comments / clinical recommendations
-
Because this involves the nasal mucosa, a joint dental + ENT review is recommended early — even if first 14 days appear uneventful — to confirm no sinus communication and to protect developing dentition.
-
Prophylactic antibiotics are not mandatory for every case but are commonly used when extraction site breaches the nasal floor or in contaminated wounds — follow your local surgical protocol.
-
Document healing with photos at baseline, 7 days, and 14 days; obtain radiograph if any persistent symptoms.
-
Educate parents about the importance of preventing nose-picking/blowing.
Visit nearest dental/ENT clinic
Find the closest clinic using your directory:
https://cebudentalimplants.com/map-dental-clinic